Personalized First-Line Treatment of Metastatic Pancreatic Neuroendocrine Carcinoma Facilitated by Liquid Biopsy and Computational Decision Support
We present the case of a 50-year-old female whose metastatic pancreatic neuroendocrine tumor (pNET) diagnosis was delayed by the COVID-19 pandemic. The patient was in critical condition at the time of diagnosis due to the extensive tumor burden and failing liver functions.
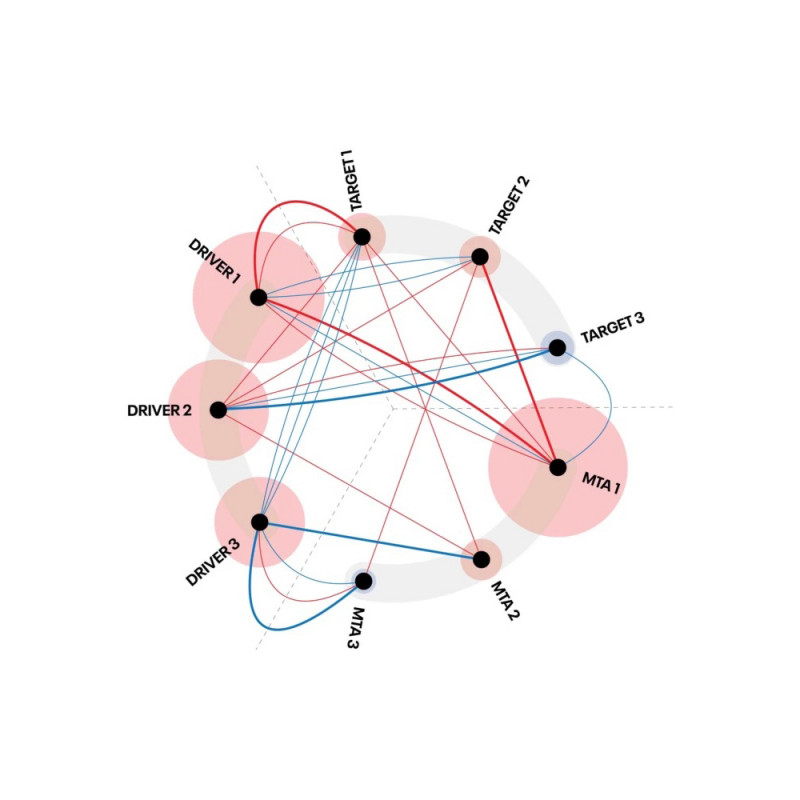
The clinical dilemma was to choose between two registered first-line molecularly-targeted agents (MTAs), sunitinib or everolimus, or to use chemotherapy to quickly reduce tumor burden. Methods: Cell-free DNA (cfDNA) from liquid biopsy was analyzed by next generation sequencing (NGS) using a comprehensive 591-gene panel. Next, a computational method, digital drug-assignment (DDA) was deployed for rapid clinical decision support. Results: NGS analysis identified 38 genetic alterations. DDA identified 6 potential drivers, 24 targets, and 79 MTAs. Everolimus was chosen for first-line therapy based on supporting molecular evidence and the highest DDA ranking among therapies registered in this tumor type. The patient’s general condition and liver functions rapidly improved, and CT control revealed partial response in the lymph nodes and stable disease elsewhere.
Conclusion: Deployment of precision oncology using liquid biopsy, comprehensive molecular profiling, and DDA make personalized first-line therapy of advanced pNET feasible in clinical settings